
I've worked in administration all my working career, from emergency services to local authority, to local press and more recently in the NHS.

I've worked in administration all my working career, from emergency services to local authority, to local press and more recently in the NHS.
My first episode came around 2007/2008 whilst I was working with the local newspaper as their advertising text inputter, which consisted of 7.5hours of almost constant typing, working to pre-set deadlines in a desk space which would make Harry Potter’s cupboard under the stairs look spacious!
As you can imagine, this was a pretty sedentary, repetitive job to be working as and, with very limited exercising outside of work and not the best BMI in the land, led to the inevitable. As most accounts have stated, this started off as cramp pains in the legs. Having had occasional calf muscle cramp pains at the time, I put the feeling in my leg down to internal bruising from the contraction and thought nothing more of it.
As the weeks went by however, the
feeling failed to subside and in fact, started to progress upwards from
the calf to my hip area and indeed switched sides from being a pain on
my right side to being on my left side. It finally came to a head when I
found it very difficult to sit or lie down without feeling waves of
pain coming from my back and the following day at work, with much
insistence from my work colleague (though I’d already booked the
appointment in the morning), I went to see my GP. The GP took one look
at me as I walked into their office and told me to go straight to our
emergency ward and I was admitted, and x-rays and scans showed clots in
both lungs (bilateral pulmonary embolisms). I was discharged and put on
Warfarin with regular INR checks.
I had two subsequent episodes of DVT after the first initial episode (1 originating from the left leg and a third occurring in the right leg as it had the first time). Most of the ‘in between’ episodes were again down to a poor dietary lifestyle and irregular-compliance with Warfarin treatment, but on occasions, my exercising regime had improved (I was walking to and from work which was a good mile and a bit and my diet had slightly improved and I’d lost 30lbs in a year).
When my third episode occurred, I was working
in a different county and travelling to work for 90 minutes by public
transport each way, which made it hard to maintain GP surgery
appointments without needing to take annual leave for the time lost
(working overtime to make up the time was also not an option due to the
building’s opening hours). It became apparent after the second episode
(which didn’t require hospital admission as I was more ‘aware’ of the
signs) that I needed to be on life-long treatment, but as a result of
missing INR checks, regularly and therefore not taking to the correct
Warfarin dose, I was switched onto Rivoroxaban and advised that this was
it; no more messing.

Well, don’t ask me why, but medication compliance slipped of my own volition, as did my exercising routine off and on (even paying monthly direct debits for a gym membership without attending!) and over the years, I ballooned to over 300lbs. Nonetheless, I travelled to Canada without any issue or pain or consequences of the long flight (luckily). After seeing the holiday photos, I decided that was it, time to get back in shape and I dedicated night after night to doing cardio and modest free/machine weight lifting at the local university gym. That year I lost 50lbs in 10 months and felt great (not as light as I was before the first episode, however) and no doubt would’ve continued on my path, had the 4th episode not happened.
The day before I was admitted into hospital, I had what, for me, was a pretty intense ‘leg day’, working all core muscle groups in the legs after my usual 1hr/1000kcal workout on the elliptical cross trainer (I LOVE the cross trainer – it’s quiet and I don’t sound like an asthmatic hippo charging in the corner of the gym as I would on a treadmill – picture if you will the glass of water scene in Jurassic Park, but at 120 ‘stomps’ a minute and that’s what my fellow gym goers’ water bottles would look like!).
I didn’t feel any soreness afterwards, so I
probably didn’t have a “my leg day almost killed me!” session (though,
now when people post this on their Instagram feeds, I think “hold on a
minute....!”), in fact, I recall watching the US Open Tennis finals
(Rafa Nadal won, woohoo!) in the evening and went to bed fine. I even
woke up in the morning fine, felt a slight twinge in my right leg as I
went downstairs but put it down to ok, leg day hangover is starting to
kick in and set off for work. Now, shamefully I would drive to work even
though I was less than a mile away from work (it’s not always the
sunniest and driest of climates in North Wales to walk daily; you could
walk to work with it being sunny in the evening and have it chuck it
down in the evening and vice versa...cough...bad excuse), BUT I was
exercising almost daily and as mentioned, was losing weight and living a
healthier lifestyle.
By the time I got near to my workplace, which fortunately in this case, was on the grounds of a general hospital, I got to the access roads and could barely feel the pedal under my right foot. I managed to park up and thought I’d hobble to A&E with pins and needles (I remember rooting through my car boot for an umbrella to use as a walking stick!). Luckily for me, 2 pharmacy nurses parked up and asked me if I was ok...I could barely walk around my car and I started to panic and get short of breath; they drove me up to A&E and after 10 minutes I was on a bed being triaged for admission (again I could barely sit comfortably in the reception area, but not feeling similar sharp pains in my chest, as my first thrombosis episode).
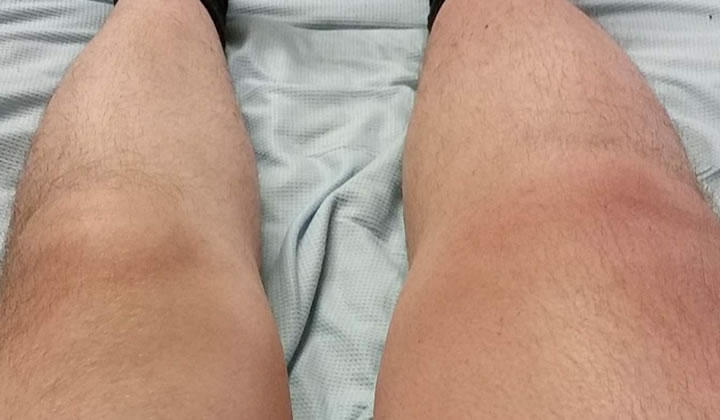
On examination, my right leg had swollen and turned purple (my left leg fine as it was in the morning) and I could barely feel any contact being made to my foot by the attending nurses and doctors. I was x-rayed and given an iodine scan all by midday and they confirmed I had another leg clot with tiny fragments in both lungs (my mother was told my leg clot was about eight inches in length extending from the main artery to the intestine).
From weighing myself that
morning, to being weighed the following day, my leg had gained
approximately 11lbs in mass (photo available). On discharge and at my
clinic appointment with the Consultant, I noted that the reason I was
given that I was prone to clots was down to a sedentary lifestyle, poor
diet and no exercise and that I needed to lose weight (I sometimes think
that even if an overweight person lost a limb, they’d still be told to
lose more weight!) and that I could understand the need for
anticoagulant treatment. This time, I was living completely the
opposite, but conceded I wasn’t taking the anticoagulant treatment and, as the
Consultant explained, fitness and diet is not the main deterrent to
getting clots, having seen many mountain peak marathon runners suffer
from blood clots.
I’ve always been curious to know what is in my physiology that causes these blood clots: particularly as on my maternal side, relatives have been more prone to anaemia, but I’ve always been told that in order to investigate this, they would have to stop the anticoagulant treatment to get a blood sample and even afterwards, it probably would not alter the treatment plan. Other than the pain of when I had the first pulmonary embolisms, the leg swelling was a visual indication of the ‘damage’ the clots were doing to my body and definitely a wake up call.
The Thrombolysis team, to their
credit were very restrained, but firm with their telling off the last
time and that I had to be more treatment-compliant this time round and
in the past 3 years, I’ve only missed two or three days of consecutive
treatment due to missing my repeat prescription date. I was due to go
back into training at the gym having enjoyed a post-Christmas
hibernation, but sadly, we went into lockdown and my gym has now been
converted into a Nightingale/Rainbow (as we’re in Wales) hospital in
response to the Covid-19 pandemic. The soonest I can get back in the gym
the better as last year I had the goal of losing weight to a ‘maximum
advised weight’ to drive supercars on the Top Gear test track, but now I
have the goal of a “meet and greet” next year with Katherine Jenkins
and I don’t want to look like a bearded big hippo next to her in the
photo (shallow Hal I know!) as well as beating my previous weight loss
target.
They sometimes refer to DVTs and PEs as silent killers, but in a weird way, I guess I’ve been fortunate (as have other contributors) to have the pain symptoms that alert me of something not being right. I think a lot of people within the sport of F1 were surprised by the death of Race Director, Charlie Whiting last year after a sudden PE, having been seen doing the circuit walkaround the day before the opening day of racing, but, unless he had ‘bearable’ symptoms, it shows how it quickly it can develop.
But, yeah, when someone ego-posts on social media that “leg-day” nearly ‘killed them’, I think these people have no idea!
It has been comforting to read some of the similar stories as to the onset of DVTs and PEs and it’s also been comforting to read on the website some of the information in connection to DVTs and COVID-19, as Public Health Boards are not very forthcoming with clear guidance if we’re at risk and absolutely should work from home or not.